Urinalysis laboratory diagnostics and its significance in addressing UTI
With around 150 million affected individuals globally, urinary tract infections (UTI) are among the most frequent bacterial infections. UTIs are accountable for millions of medical consultations and put significant burden on healthcare systems and societies [1,2].
Despite its costly and time-consuming nature, urine culture remains the gold standard in UTI diagnostics and accounts for up to 40% of the overall requested cultures in a lab [3]. This workflow can clog up resources in the laboratory as well as cause a gap in communication between the lab and clinicians, which can trickle down to patients and treatment methods. 80% of suspected UTI samples turn out to be negative, therefore a fast and reliable method to exclude UTI can be a driver for laboratory workflow improvements and antimicrobial stewardship [4].
Rule out UTI in less than a minute
With a diagnostic performance of 0.973 (AUC), the UF-series can provide quantitative information on bacteriuria in less than a minute. A recent investigation of different cut-off values revealed a bacteria count of ≥ 58 cells/μL as the most sensitive value for ruling out urinary tract infections with a sensitivity of 99.4 % (NPV 99.7 %) and a specificity of 78.2 % (PPV 65.4 %) [5].
The UF-series utilises fluorescence flow cytometry, which is a technology that can also benefit the antibiotic susceptibility testing (AST) process by screening samples. that negative UTI samples can be ruled out with this technology, culture plating and general workload can be optimised. There is also the possibility to utilise bacteria information flags which can predict positive samples containing Gram negative bacteria for Direct Antibiotic Susceptibility Testing (dAST). dAST on the positive urine samples can reduce response time for antibiotic profile by up to 24 hours, and thus contribute to reduced empiric use of antibiotic and shorter overall treatment. [6]
![[.SE-se Sweden (swedish)] UF-series utilises fluorescence flow cytometry [.SE-se Sweden (swedish)] UF-series utilises fluorescence flow cytometry](/fileadmin/_processed_/8/a/csm_laser_scanning_d7c7ae5972.png)
BACT info
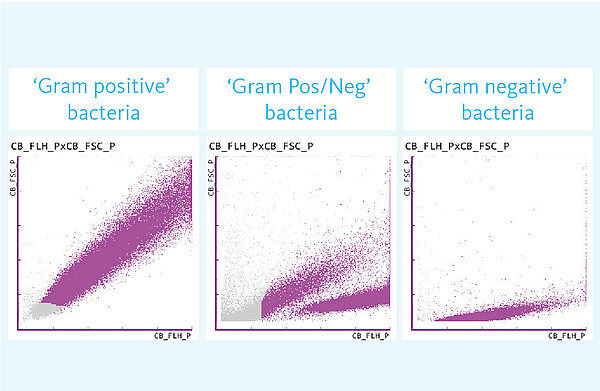
The BACT-info flag provides additional information on the Gram dye affinity for samples positive for bacteriuria. Suspicious samples are highlighted with any of the following flags:
- Gram Positive?
Based on the distribution, it can be inferred that Gram-positive bacteria are present.
- Gram Negative?
Based on the distribution, it can be inferred that Gram-negative bacteria are present.
- Gram Pos/Neg?
Based on the distribution, it can be inferred that Gram-positive and Gram-negative bacteria are present.
- Unclassified
The class does not become clear from the distribution.
Gram-positive bacteria are detected with a sensitivity of 78% and a specificity of 96%, whereas for Gram-negative bacteria, both the sensitivity and specificity reach 89%. This might allow an early initiation of antibiotic UTI therapy and more targeted follow-up diagnostics [5].
RBC (red blood cells)
Infections of the urinary tract can trigger inflammation and irritation on the urothelium that can cause haematuria. Urinary particle analysis can detect urinary RBC and distinguish between isomorphic and dysmorphic RBC.
WBC (white blood cells)
Infections of the urinary tract cause urothelial inflammation that can trigger leucocyturia that can reliably be detected from the urinary sediment.
RTEC (renal tubular epithelial cells)
Renal tubular epithelial cells have been demonstrated to act as a supportive parameter to distinguish between upper and lower urinary tract infection, thereby the classical marker of UTI [7].
YLC (yeast-like cells)
Yeast-like cells bear the potential to exclude funguria and to initiate a targeted diagnostic approach [8].
Beyond urinalysis
Antibiotic susceptibility testing to address UTI workflow
In addition, antibiotic susceptibility testing (AST) is an important laboratory test to initiate a targeted antibiotic treatment and fight antimicrobial resistance (AMR). There are newer technologies under development to improve and speed up the AST process. One technology measures the growth rate of bacterial cells in real time through microfluidics and image analysis methods. A sample is loaded onto a microfluidic chip and any bacteria present are caught in bacteria-sized traps. The trapped bacteria are monitored, whereby the loading time gives an estimate of the density of bacteria in the sample. Bacterial growth is monitored in each trap, some of which contain a candidate antibiotic. The average growth rates are calculated in real time and the bacteria are considered susceptible if its growth is duly inhibited.
Still want to know more?
We have a collection of further materials that allow you to dive deeper into the topic of urinary tract infections, urinalysis workflow and related topics. Check out our white paper, webinars and interviews with experts to get more information.
References
- Stamm WE, Norrby SR (2001): Urinary tract infections: Disease paranormal and challenges. J Infect Dis 183 (Suppl. 1) S1–S4.
- Foxman B (2014): Urinary Tract Infection Syndromes: Occurrence, Recurrence, Bacteriology, Risk Factors and Disease Burden. Infect Dis Clin North AM 28(1):1–13.
- Wilson and Gaido (2004) Laboratory Diagnosis of Urinary Tract Infections in Adult Patients. Clinical Infectious Disease 38:1150–8
- Keller (2019) Ein neuer Schritt zur schnelleren Urinanalytik. Sysmex xtra 02/2019:50-52
- De Rosa et al. (2018): Evaluation of the new Sysmex UF-5000 fluorescence flow cytometry analyser for ruling out bacterial urinary tract infection and for prediction of Gram-negative bacteria in urine cultures. Clinica Chimica Acta 484:171–178
- Gilboe, H. M., Reiakvam, O. M., Aasen, L., Tjade, T., Bjerner, J., Ranheim, T. E., & Gaustad, P. (2021). Rapid diagnosis and reduced workload for urinary tract infection using flowcytometry combined with direct antibiotic susceptibility testing. Plos one, 16(7), e0254064.
- Oyaert et al. (2020) Renal tubular epithelial cells add value in the diagnosis of upper urinary tract infection. Clin Chem Lab Med 58(4):597-604
- Song et al. (2018) Selection of unnecessary urine cuture specimens using Sysmex UF-5000 urine flow cytometer. Ann Clin Microbiol 21:75-79