Scientific Calendar October 2021
Ruling out post-prostatectomy urinary tract infection
What are potential urinalysis findings post-surgery, for example post-prostatectomy?
Microalbuminuria
Isomorphic RBC
Dysmorphic RBC
Pyuria
Casts
Renal tubular epithelial cells
Congratulations!
That's the correct answer!
Sorry! That´s not completely correct!
Please try again
Sorry! That's not the correct answer!
Please try again
Notice
Please select at least one answer
Scientific background
With more than 150 million reported cases annually, urinary tract infections (UTI) belong to the most common infections globally [1]. They are one of the leading nosocomial infections, accounting for up to 12% of all hospital-acquired infections. Catheterisation is a main driver of catheter-associated UTI (CAUTI) and can thus complicate treatment of hospitalised patients [2].
The partial or complete surgical removal of the prostate (prostatectomy) is a common medical intervention in context of benign prostatic hypertrophy and prostate cancer. Enlargement of the prostate may cause diverse urinary complaints, including urinary retention as well as obstructive and irritative symptoms. Urinary tract infection can have impact on the prostatectomy in a pre- or postoperative manner. Preoperative lower UTI can be observed in up to 15% of prostatectomy patients – a common complaint among middle-aged men. Postoperative UTI is detected in up to 7.5% of prostatectomy patients and may be a result of catheterisation [3].
Prostatectomy is reported with positive early postoperative outcomes, only showing complications in 17% of the respective cases. With an incidence of 5%, urinary tract infections comprise the second most frequent postoperative event [4].
Furthermore, a prostatectomy can cause an inflammatory condition through the surgical intervention itself. However, excluding the additional UTI can help differentiate infections and inflammations and thus influence treatment decisions.
Numerical results
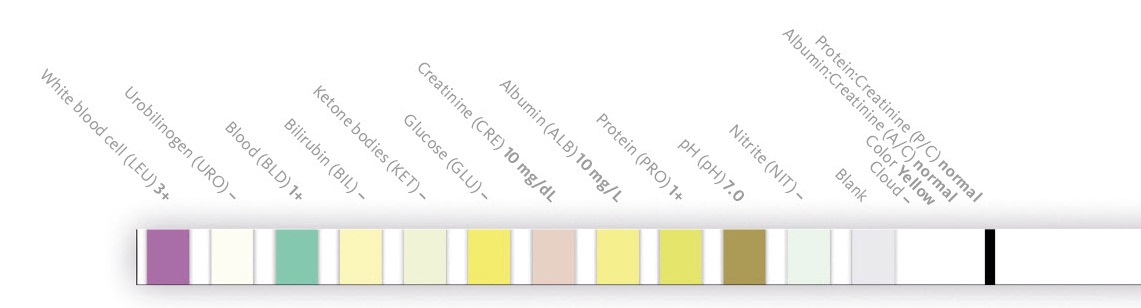
Following a prostatectomy, a catheterised patient showed slight symptoms of a lower urinary tract infection. A urine specimen was initially investigated by automated test strip analysis using a Meditape 11A test strip on the UC-3500. The specimen was negative for nitrite test but revealed the presence of pyuria and haematuria. Since a negative nitrite test is not sufficient to rule out UTI if UTI-related symptoms are present, a subsequent analysis for urinary particles was conducted.
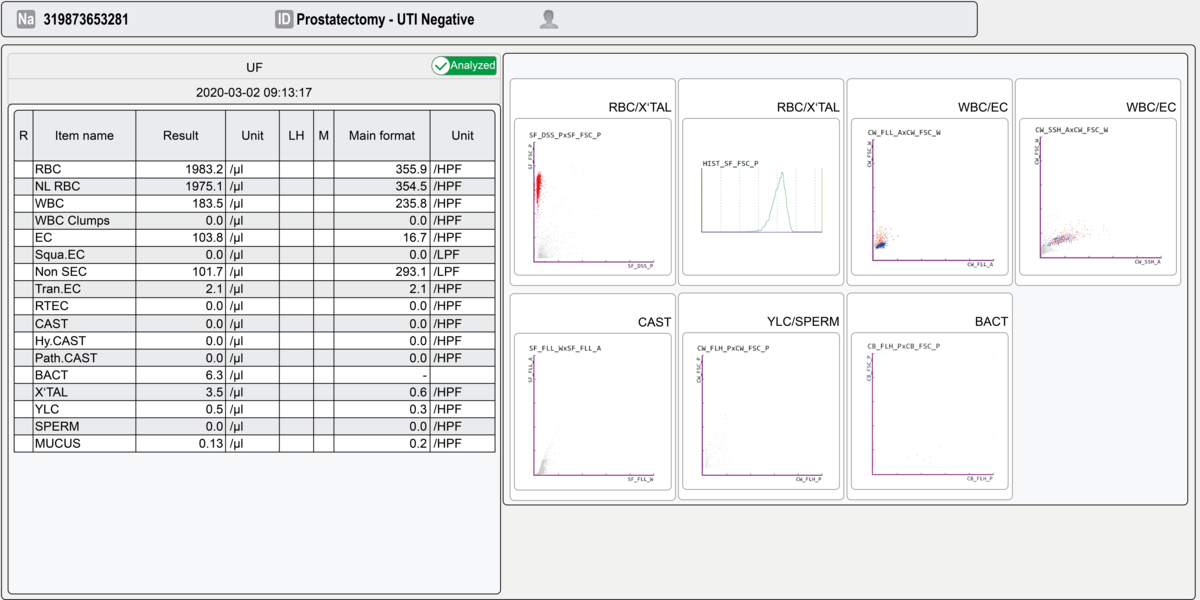
The flow cytometric detection of particles through the UF-5000 confirmed the pyuria with 183.5 WBC/µL and haematuria with1983.2 RBC/µL. Moreover, the scattergram distribution for the RBC highlights the presence of isomorphic RBC, indicating a bleeding in the lower urinary tract. The particle analysis did not reveal any bacterial or fungal cells, therefore allowing the confident exclusion of bacteriuria and the direct rule-out of UTI [5]. Both the pyuria and the haematuria can thus be a result of the catheterisation and the associated urothelial irritation, but are also a common, non-pathological postoperative finding among the prostatectomy patients [6].
The present patient case demonstrates the potential of the UF-series to rule out urinary tract infection in a post-prostatectomy condition to avoid unnecessary treatment and diagnostic procedures.
References
[1] Foxman B (2014): Urinary Tract Infection Syndromes: Occurrence, Recurrence, Bacteriology, Risk Factors and Disease Burden. Infect Dis Clin North AM. 28(1):1–13.
[2] Khan HA et al. (2017): Nosocomial infections: Epidemiology, prevention, control and surveillance. Asian Pac J Trop Biomed. 7(5):478-482.
[3] Pourmand G et al. (2010): Urinary infection before and after prostatectomy. Saudi J Kidney Dis Transpl. 21(2):290-4.
[4] Gratzke C et al. (2007): Complications and early postoperative outcome after open prostatectomy in patients with benign prostatic enlargement: Results of a prospective multicenter study. J Urol. 177(4):1419-22.
[5] Gilboe HM et al. (2021): Rapid diagnosis and reduced workload for urinary tract infection using flowcytometry combined with direct antibiotic susceptibility testing. PLoS One 6(7):e0254064.
[6] Olvera-Posada D et al. (2013): Natural history of pyuria and microhematuria after prostate surgery. Actas Urol Esp. 37(10):625-9.